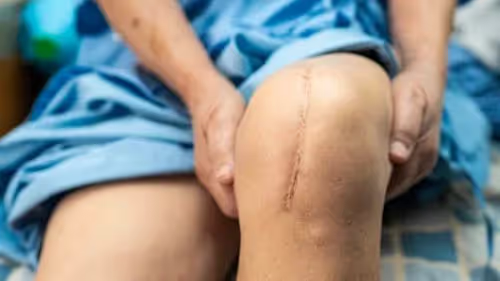
A knee replacement is a surgical procedure that replaces the damaged or worn-out knee joint with an artificial joint, called a prosthesis. The procedure is usually performed in people with severe knee arthritis or other knee conditions that cause chronic pain and disability.
While knee replacement surgery can improve joint function and reduce pain, it is also associated with post-operative discomfort and swelling. To manage these symptoms, many doctors recommend the use of ice therapy after knee replacement surgery.
Why does ice help after knee replacement surgery?
Ice therapy, also known as cryotherapy, is a common treatment for managing pain, inflammation, and swelling after knee replacement surgery. Ice helps in reducing pain. Ice stimulates the nerve endings in the knee and reduces pain signals to the brain. This can help alleviate discomfort and make it easier to perform physical therapy exercises. Ice helps with decreasing inflammation. Knee replacement surgery causes inflammation in the knee joint and surrounding tissues. Ice therapy can help reduce inflammation by constricting blood vessels and limiting the flow of fluid to the area. Ice helps in preventing swelling. Swelling is a common side effect of knee replacement surgery. Ice therapy can help prevent swelling by reducing the amount of fluid that accumulates in the knee joint. Ice can help improve circulation. Although ice constricts blood vessels, it can also promote circulation by causing the blood vessels to expand and contract. This can help bring oxygen and nutrients to the knee joint, which can aid in the healing process.
The science behind icing.
The human body is equipped with a complex nervous system that is responsible for transmitting and processing various types of sensory information, including pain. There are different types of nerve fibers that are involved in pain and sensation, including alpha nerve fibers and delta nerve fibers. In this article, we will explore the differences between these two types of nerve fibers and their roles in pain and sensation.
Alpha Nerve Fibers
Alpha nerve fibers, also known as A fibers, are a type of large, myelinated nerve fibers that are responsible for transmitting information related to touch, pressure, temperature and vibration. These fibers have a diameter of 5-20 micrometers and can transmit information at speeds of up to 120 meters per second.
Because of their large size and fast transmission speed, alpha nerve fibers are important for transmitting information related to fast sensations. For example, if you touch a hot stove, the alpha nerve fibers in your skin will quickly send a signal to your brain, triggering a reflex to withdraw your hand. The same goes for cold temperatures. If you place a cold ice pack on your knee, the alpha nerve fibers are activated.
However, alpha nerve fibers are not involved in transmitting information related to dull, aching pain. This type of pain is transmitted by another type of nerve fiber called the delta nerve fiber.
Delta Nerve Fibers
Delta nerve fibers, also known as Aδ fibers, are a type of small, myelinated nerve fibers that are responsible for transmitting information related to dull, aching pain, which is very common after a knee replacement. These fibers have a diameter of 1-5 micrometers and can transmit information at speeds of up to 30 meters per second. They are much slower than alpha nerve fibers.
Because of their smaller size and slower transmission speed, delta nerve fibers are not as effective at transmitting information related to touch, temperature pressure as alpha nerve fibers. However, they are important for transmitting information related to pain that is caused by mechanical or chemical stimuli.
Delta nerve fibers are activated when the skin is pierced, cut, or burned, or when chemicals are released in response to inflammation or infection.

The Role of Alpha and Delta Nerve Fibers with Icing
The transmission of pain signals involves a complex interaction between different types of nerve fibers and the spinal cord and brain. When a painful stimulus is detected, sensory nerve fibers in the affected area transmit signals to the spinal cord, where they synapse with other neurons that relay the signal to the brain.
The type of nerve fiber that is activated by the painful stimulus determines the nature of the pain that is perceived. Temperature, pressure and touching pain or sensations is typically transmitted by alpha nerve fibers, while dull, aching pain is transmitted by a different type of nerve fiber called the delta fibers
So what does this have to do with icing my knee after a knee replacement?
Because alpha fibers are so much faster than delta fibers, they actually interrupt the pain signal. When you place ice on your aching knee, you will quickly activate the alpha nerve fibers (temperature, touch and pressure) causing the delta nerve fibers (pain) to be interrupted and suppressed. This is what we call Gate Theory.
An example: When you bump your elbow on something hard, what do you immediately do to help the pain? You rub your elbow. When you rub your elbow you are activating the alpha nerve fibers (temperature, touch and pressure) causing the delta nerve fibers (pain) to be interrupted and suppressed. This is because the alpha nerve fibers are faster and they get to the brain before the delta nerve fibers can - causing less pain for you.
This same theory applies to icing your knee.
How to use ice therapy after knee replacement surgery
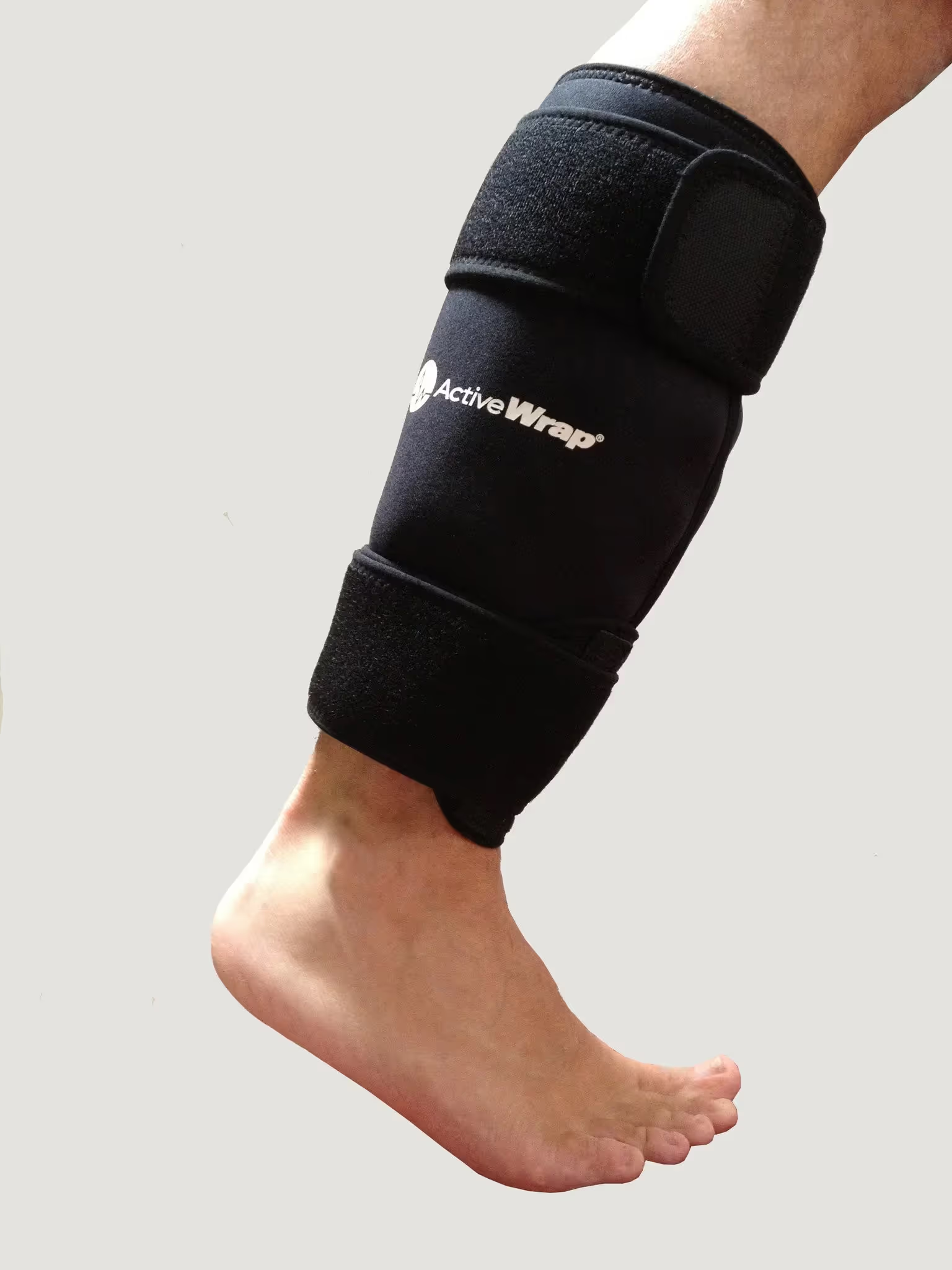
If your doctor recommends ice therapy after knee replacement surgery, it is important to use it correctly to avoid injury or discomfort. Here are some tips for using ice therapy effectively:
- Use ice packs or ice machine: Ice packs are the most common way to apply ice therapy after knee replacement surgery. You can purchase pre-made ice packs or make your own by placing ice cubes in a plastic bag or wrapping them in a towel. Most knee replacement patients opt to use a ice machine instead of ice packs because it stays colder causing more pain relief.

- Best ice pack after knee replacement- use code DRSAM10 for 10% off
- Apply ice for 20 minutes at a time: To avoid damaging the skin or tissues, it is recommended that you apply ice for no more than 20 minutes at a time. Although some surgeons keep the ice on your knee right after surgery for 24 hours, but once you get home, you will want to decrease the icing time. After 20 minutes, remove the ice pack and wait at least 20-30 minutes before reapplying.
- Use a barrier between your skin and the ice pack: Direct contact between the ice pack and your skin can cause skin irritation or frostbite. To prevent this, use a thin towel or cloth between your skin and the ice pack.
- Elevate your knee: Elevating your knee above your heart can help reduce swelling and improve circulation. When using ice therapy, prop your knee up on a pillow or cushion to keep it elevated.
- Use ice therapy as directed by your doctor: Your doctor will provide specific instructions on how often and how long to use ice therapy after knee replacement surgery. It is important to follow these instructions to ensure that you are using ice therapy safely and effectively.
How Does Ice Help Inflammation and Decrease Scar Tissue Formation?
When an injury occurs, the body's immune system is activated to respond to the injury and promote healing. The first stage of inflammation is characterized by the release of various chemicals, including histamine, prostaglandins, and cytokines, from damaged tissues and immune cells.
These chemicals cause blood vessels in the injured area to dilate (aka open up), which increases blood flow to the site of the injury. This increased blood flow results in redness, warmth, and swelling in the affected area. The dilation of blood vessels also allows white blood cells to migrate to the site of the injury to begin the process of tissue repair.
Although it is imperative for the blood vessels to open up after an injury to allow all the inflammatory cells in to heal the injured area, these cells will cause a variety of unpleasant symptoms such as pain, aching, throbbing and stiffness. All of these symptoms cause you the inability to sleep and do your physical therapy exercises and stretches. So we have to control this inflammatory process with ice and elevation.
White Blood Cells and Tissue Repair
White blood cells, also known as leukocytes, are an important component of the immune system and play a crucial role in tissue repair and healing. There are several types of white blood cells, including neutrophils, monocytes, and lymphocytes, each of which plays a specific role in the inflammatory response.
Neutrophils are the first type of white blood cell to arrive at the site of injury. These cells are attracted to the area by chemical signals released by damaged tissues and immune cells. Once at the site of injury, neutrophils engulf and destroy bacteria, debris, and other foreign substances through a process called phagocytosis.
Monocytes, another type of white blood cell, also play an important role in tissue repair. When monocytes enter the injured area, they differentiate into macrophages, which are responsible for clearing away dead cells, debris, and other waste products from the site of the injury.
Lymphocytes, the third type of white blood cell, are involved in regulating the immune response and promoting tissue repair. B cells produce antibodies that help neutralize pathogens and prevent further infection, while T cells help coordinate the immune response and promote tissue repair.
Fibroblasts are a type of cell found in connective tissue that are responsible for producing the extracellular matrix (ECM), which is the non-cellular component of tissue that provides structural support, elasticity, and mechanical strength. When an injury occurs, such as a cut or a burn, fibroblasts play a crucial role in the healing process by producing new collagen fibers to repair the damaged tissue. However, in some cases, fibroblasts can cause the formation of scar tissue, which can be problematic.
Over time, as tissue repair and healing progress, the inflammatory response begins to subside. The blood vessels in the affected area return to their normal size, and the swelling, redness, and warmth gradually dissipate. However, after a knee replacement, this inflammatory response last for a long time due to the extensive nature of the surgery. Not only was the skin damaged, but the muscles, tendons, ligaments and bone.
The Formation of Scar Tissue
Scar tissue is a type of connective tissue that forms in response to injury or inflammation. It is composed of collagen fibers, which are produced by fibroblasts, and can have a different appearance and texture than the surrounding tissue. Scar tissue is generally less flexible and elastic than healthy tissue, which can lead to functional impairments, such as reduced range of motion or joint stiffness.
The formation of scar tissue occurs when fibroblasts become activated in response to injury or inflammation. Once activated, fibroblasts migrate to the site of injury and begin to produce collagen fibers to repair the damaged tissue. In some cases, however, the fibroblasts continue to produce collagen even after the tissue has been repaired, leading to the formation of excess scar tissue.
Factors that Influence Scar Tissue Formation
Several factors can influence the formation of scar tissue, including the type and severity of the injury, the individual's age and genetics, and the presence of underlying health conditions. For example, wounds that take longer to heal or that become infected are more likely to develop scar tissue. Additionally, individuals with a genetic predisposition to scarring may be more prone to developing excess scar tissue.
Reducing Scar Tissue
Keeping up with your physical therapy exercises and stretches is key to ensuring scar tissue does not form densely within the knee causing the knee not to bend or straighten fully. Having an educated physical therapist that has many years of experience with treating knee replacement patients is also very important. If you are concerned with your currently level of care, please enroll in one of the course on http://www.SUCCEEDCOURSES.com
Elevating and icing the knee will also help the knee not form as much scar tissue because we are reducing the amount of fibroblasts in the knee.
Alternatives to ice therapy
Some individuals may not have relief from icing and need other options. While ice therapy is a common treatment for managing pain and swelling after knee replacement surgery, there are other treatments that may be effective as well. Here are some alternatives to ice therapy:
Heat therapy: Heat therapy can help relax the muscles in the knee joint and improve circulation. Please check with your surgeon before applying heat to your knee. 99% of the time applying heat to the muscles aroudn your knee is okay, but if you have had complications after your surgery, this may not be appropriate. You can use a heating pad or even take a warm bath to apply heat therapy to your knee. Baths are recommended after the incision is fully healed between 4-6 weeks after surgery.
Compression therapy: Compression therapy involves using a compression bandage or stocking to apply pressure to the knee joint. This can help reduce swelling and improve circulation. Compression is very effective in reducing swelling. Combining compression, ice and elevation would be the best option.
Medications: Your doctor may prescribe medications to manage pain and inflammation after knee replacement surgery. These may include over-the-counter pain relievers, nonsteroidal anti-inflammatory drugs (NSAIDs), or prescription opioids.
Physical therapy: Physical therapy is an important part of the recovery process after knee replacement surgery. Your physical therapist will work with you to develop an exercise program that can help improve strength, flexibility, and range of motion in your knee joint. Physical therapy can also help reduce pain and swelling after surgery.
Massage therapy: Massage therapy can help improve circulation and reduce tension in the muscles surrounding the knee joint. A licensed massage therapist or physical therapist can use techniques such as deep tissue massage, or myofascial release to help manage pain and improve mobility after knee replacement surgery.

.avif)